Urine EtG testing is one of the most common ways programs check for recent alcohol use. It’s used in addiction treatment, probation monitoring, workplace and occupational health screening, and other alcohol abstinence monitoring plans.
But most confusion doesn’t come from EtG itself—it comes from the cutoff. A “positive” at one cutoff can be a “negative” at another, even when the measured number is the same.
Quick short answer
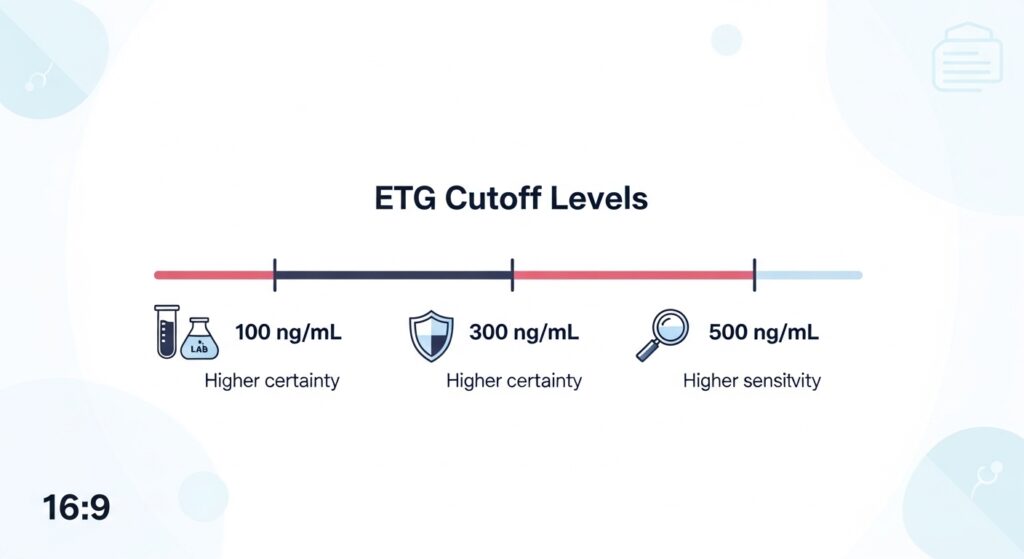
An EtG cutoff is the threshold (like 100, 300, or 500 ng/mL) used to report a urine EtG result as negative or positive. Lower cutoffs detect more recent/light alcohol exposure but increase incidental-exposure positives; higher cutoffs reduce disputes but may miss light or older drinking.
What is EtG (ethyl glucuronide), and what is it not?
Ethyl glucuronide (EtG) is an ethanol metabolite—a byproduct your body forms after alcohol is in your system. Many tests also include ethyl sulfate (EtS), another ethanol metabolite that can support interpretation.
EtG is useful because alcohol itself can disappear quickly, while EtG may remain detectable longer in urine.
EtG is not:
- A blood alcohol concentration (BAC) substitute
- Proof of intoxication or impairment
- A precise calculator of “how many drinks” you had
- A stopwatch that tells an exact time of last drink
EtG is best used as a recent-exposure marker interpreted alongside the cutoff, timing, and testing conditions.
The three most common EtG cutoffs: 100 vs 300 vs 500 ng/mL
Programs typically choose a cutoff based on a tradeoff: sensitivity vs specificity.
- Sensitivity: catches more true drinking (especially lighter use or farther back)
- Specificity: reduces “noise” from incidental exposure (mouthwash, sanitizer) and lowers disputed positives
At-a-glance comparison table
| Cutoff (ng/mL) | Sensitivity (detects more) | Specificity (fewer incidental positives) | Best fit for | Main downside |
|---|---|---|---|---|
| 100 | Highest | Lowest | Strict abstinence monitoring, early relapse detection | More vulnerable to incidental exposure and edge-case positives |
| 300 | Balanced | Balanced | Programs wanting a middle ground | Still requires context; not dispute-proof |
| 500 | Lowest | Highest | Workplace/legal settings prioritizing fewer disputes | Can miss light drinking or older use |
Which is strictest?
100 ng/mL is the strictest cutoff because it’s the most sensitive and most likely to flag light drinking or older exposure. 500 ng/mL is least strict in detection terms but often chosen to reduce incidental-exposure positives.
What each cutoff level means in real life
1) EtG cutoff 100 ng/mL: “high sensitivity”
A 100 ng/mL cutoff is designed to detect more alcohol exposure scenarios. That can be helpful in strict monitoring—especially when the goal is “any use matters.”
Common use cases
- Certain addiction treatment or recovery monitoring plans
- High-accountability abstinence contracts
- Some clinical monitoring contexts where early detection is prioritized
What people misunderstand
At 100 ng/mL, very small signals can matter. This is where questions like “I used mouthwash—will I fail?” often show up, because the cutoff leaves less margin for incidental exposure.
2) EtG cutoff 300 ng/mL: “middle ground”
300 ng/mL is a practical compromise many programs use to balance detection with fewer incidental positives than 100.
Why 300 is often overlooked (and why it matters)
Most online content argues about 100 vs 500, but 300 is frequently the real-world “policy compromise.” If you’re writing or managing a program, 300 can reduce disputes while still detecting more than 500.
Common use cases
- Outpatient monitoring
- Programs aiming for a balanced approach
- Some occupational health workflows where risk tolerance is moderate
3) EtG cutoff 500 ng/mL: “higher specificity”
500 ng/mL is often chosen when the program wants fewer positives linked to incidental exposure, and fewer contested results.
Some major lab workflows in the US/Canada use a 500 ng/mL threshold and may require EtS (for example, EtS ≥100 ng/mL) to support a reported positive. That “paired marker” approach is designed to reduce misinterpretation.
Common use cases
- Workplace testing and safety-sensitive job policies
- Certain legal/probation contexts focused on defensibility
- Situations where chain-of-custody and confirmation are prioritized
Does “EtG 250” mean if cutoff is 500?
If your measured EtG is 250 ng/mL and the program cutoff is 500, the report is usually negative—but it still indicates a detectable signal. In strict programs, that number may trigger questions about timing or incidental exposure, even if “negative.”
Detection windows: the part everyone wants, and why it’s tricky
People search “EtG 48 hours,” “EtG 72 hours,” or “EtG 80 hours” because they want certainty. The honest answer is: detection depends on dose, timing, metabolism, urine concentration, and the cutoff.
Here’s a safer, more accurate way to think about it:
- Lower cutoffs (100) generally detect more scenarios and can detect alcohol exposure farther back than higher cutoffs.
- Higher cutoffs (500) tend to detect heavier or more recent exposure better and may miss light or older exposure.
What a urine EtG result cannot prove (important in high-stakes situations)
- It usually can’t prove exactly how much alcohol was consumed
- It usually can’t prove exactly when alcohol was consumed
- It cannot prove impairment at work or while driving
If the question is impairment, programs typically use breath alcohol testing or blood ethanol.
Why false positives and “disputed positives” happen
EtG is a strong tool, but it’s not immune to problems. The biggest controversy is incidental exposure (sometimes called extraneous exposure).
Common incidental exposure sources
- Alcohol-based hand sanitizer (frequent use, heavy exposure)
- Mouthwash and breath sprays
- Some over-the-counter products (certain cough syrups, extracts)
- Occupational exposures (certain healthcare or industrial environments)
This is why very low positives can be difficult to interpret in isolation.
Can sanitizer or mouthwash cause a positive?
They can contribute to low-level EtG signals in some cases, especially with frequent exposure. Risk is higher at lower cutoffs (like 100). Programs reduce disputes by using confirmation testing, reviewing exposure history, and sometimes requiring EtS alongside EtG.
How EtG testing works: screening vs confirmation (and why EtS matters)
Not all EtG tests are the same. Two pieces matter a lot:
- Testing method
- Whether the test includes EtS
Immunoassay screening vs LC-MS/MS confirmation
Many systems use an initial immunoassay screen. It’s efficient, but it’s not the final word in many high-stakes settings.
For defensible results, labs may confirm using chromatography / mass spectrometry, commonly LC-MS/MS (liquid chromatography–tandem mass spectrometry). LC-MS/MS is more specific and is the preferred method for confirmation in disputed or high-consequence cases.
Why some tests include EtS (ethyl sulfate)
EtS is another ethanol metabolite. When EtG and EtS move together, interpretation becomes stronger. Some lab policies and programs use EtS thresholds specifically to reduce uncertain interpretations.
Short answer (≤45 words): why do some labs require EtS too?
Because EtS can strengthen interpretation when EtG alone is borderline. Paired EtG/EtS reporting can reduce disputes caused by specimen issues, incidental exposure, or degradation concerns, especially when the outcome affects employment, legal status, or medical monitoring.
How to interpret an EtG report (step-by-step)
Use this simple process before you panic or celebrate:
- Identify the cutoff: 100, 300, or 500 ng/mL
- Check whether EtS is included and its threshold (if reported)
- Confirm the method: immunoassay screening vs LC-MS/MS confirmation
- Apply context:
- Time since last drink (if any)
- Incidental exposure (mouthwash, sanitizer, medications)
- Whether the sample was dilute (see creatinine)
- Match to program policy: the program sets the consequence, not the number alone
Practical interpretation bands (common SERP framing)
Many programs describe ranges roughly like:
- “Very low positive”: about 100–500 ng/mL
- “Low positive”: about 500–1000 ng/mL
- “High positive”: >1000 ng/mL
These bands are not universal law. They’re a way to talk about context—especially the “very low” zone where incidental exposure becomes a bigger conversation.
For individuals: what to do if you get a low-level positive
If your result is in the “very low” range (or near your cutoff), your next steps matter.
If your situation is high-stakes (job, probation, court, licensing)
- Ask if the test was confirmed by LC-MS/MS
- Ask whether EtS was included
- Ask whether chain of custody was used (especially workplace/legal)
- Document potential incidental exposures in the 1–3 days before the test:
- brands/types of mouthwash
- sanitizer frequency
- medications or extracts containing alcohol
- Do not rely on online timelines that promise “safe after X hours”
If you are monitoring for recovery or personal goals
A low-level positive can still be useful information. Focus on:
- consistency of results over time
- avoiding exposure that creates confusing signals
- discussing thresholds with your provider if the goal is relapse prevention vs dispute avoidance
For employers, clinics, and programs: choosing a cutoff (policy rubric)
If you’re designing a policy, the “right” cutoff depends on your goal.
Decision framework: what are you optimizing for?
Choose 100 ng/mL when:
- Your priority is detecting any use early
- The environment can tolerate more follow-up and context review
- The program includes confirmatory testing and clear communication about incidental exposure
Choose 300 ng/mL when:
- You want a middle ground between detection and fewer disputes
- You want a practical threshold without going to the most conservative option
Choose 500 ng/mL when:
- Your priority is fewer contested positives
- You need defensible outcomes with chain-of-custody workflow
- The program is more focused on recent/heavier exposure signals
Pros and cons summary
- 100: best detection coverage; higher edge-case positives
- 300: balanced; still requires context
- 500: fewer disputes; can miss light/older drinking
Where to get an EtG test (global, with US/Canada + UK/EU context)
Even though the topic is informational, many readers also want “EtG test near me” options.
Common provider types
US/Canada
- National lab networks (often ordered through draw sites)
- Occupational health clinics
- Independent drug testing centers
UK/EU
- Occupational health providers
- Private pathology labs / hospital labs
- Workplace testing vendors
Questions to ask any testing provider near me
- “What cutoff do you use: 100, 300, or 500 ng/mL?”
- “Do you include EtS?”
- “Is confirmation by LC-MS/MS included if needed?”
- “Do you provide chain of custody?”
- “What is the typical turnaround time?”
Typical pricing (wide range; depends on method and custody)
Costs vary by country, provider type, and whether you need:
- EtG only vs EtG + EtS
- screening only vs LC-MS/MS confirmation
- standard collection vs chain of custody (often higher)
As a broad guide, consumer-facing EtG urine tests in the US/Canada market may be priced from under $100 to a few hundred dollars depending on confirmation and custody requirements. UK/EU private testing can also vary widely based on provider and documentation.
Related Tools
We offer multiple tools to complement your ETG tracking:
- ETG Calculator – Enhanced calculations for precise monitoring.
- ETG Half-Life Calculator – Understand how long ETG stays in your system.
- ETG Calculator Accurate: Understanding Its Use – Learn how ETG levels are estimated.
- Alcohol Testing and Safety – Educational blog for safe drinking habits.
These tools are interconnected to give you a complete and reliable understanding of alcohol metabolism and ETG detection.
Common mistakes that create confusion
- Mistaking EtG for impairment testing (it isn’t)
- Not knowing your cutoff (100/300/500 changes everything)
- Ignoring EtS and confirmation method
- Over-hydrating to “beat” a test: dilution can complicate interpretation and may be detected via creatinine
- Assuming one timeline fits everyone (“I’m safe after 48 hours”)
Alternatives to EtG (when another tool fits better)
If your goal isn’t “recent exposure in the last few days,” consider alternatives:
- Breath alcohol: best for immediate, impairment-relevant questions
- Blood ethanol: acute exposure
- PEth (phosphatidylethanol): longer-term pattern monitoring (weeks)
- CDT (carbohydrate-deficient transferrin): heavier/chronic pattern monitoring in some contexts
EtG is excellent for recent exposure monitoring, but it isn’t a one-size-fits-all biomarker.
Quick takeaway: picking the right interpretation lens
Before you interpret a number, always anchor to four facts:
- cutoff (100/300/500)
- EtS included or not
- screening vs LC-MS/MS confirmation
- program policy and real-world context
That combination is what turns a lab result into a fair conclusion.
7+ FAQs (human readable)
1) What EtG level is considered positive?
It depends on the program cutoff. Many use 100, 300, or 500 ng/mL. A result above the cutoff is typically reported positive; below is reported negative. The same measured value could be negative at 500 and positive at 100.
2) Is 100 ng/mL EtG a fail?
At a 100 ng/mL cutoff, results at or above 100 are typically reported positive. It’s a strict cutoff designed to detect more alcohol exposure, including lighter use. It may also increase the chance of low-level positives from incidental exposure.
3) What does a 500 ng/mL EtG cutoff mean?
A 500 ng/mL cutoff generally means the lab reports positive only when EtG is 500 or higher. Many programs choose it to reduce disputed positives and incidental-exposure issues, but it may miss lighter or older exposure compared with lower cutoffs.
4) Can mouthwash cause a positive EtG test?
It can contribute to low-level EtG signals in some situations, especially with frequent use and lower cutoffs like 100. If your situation is high-stakes, ask about EtS and LC-MS/MS confirmation and document potential incidental exposure.
5) How long does EtG stay in urine at 100 vs 500?
There isn’t a single guaranteed window. In general, 100 ng/mL detects more scenarios and can detect alcohol exposure farther back than 500 ng/mL, while 500 is more likely to reflect heavier or more recent exposure. Timing varies person to person.
6) Why do some tests include EtS with EtG?
EtS (ethyl sulfate) is another ethanol metabolite. Including EtS can strengthen interpretation, especially for borderline results, specimen issues, or disputed positives. Some lab workflows may require EtS above a threshold to support a reported positive.
7) What should I do if I get a “very low positive” EtG result?
First, confirm the cutoff and whether the result was confirmed with LC-MS/MS. Check if EtS was measured. Then document possible incidental exposures (mouthwash, sanitizer, medications) and follow your program’s dispute or review process if consequences are involved.
8) Can drinking lots of water make EtG negative?
Over-hydration may dilute urine and complicate interpretation, but it can also raise red flags. Many testing workflows assess dilution using markers like creatinine. Dilution isn’t a reliable or safe plan, especially in monitored programs.
Conclusion
EtG cutoff levels—100, 300, and 500 ng/mL—are not just technical details. They decide how sensitive the test is, how likely a low-level signal becomes a reportable positive, and how much room there is for incidental exposure and disputes.
If you remember one thing, make it this: interpret the result through the cutoff, the method (screening vs LC-MS/MS), and whether EtS is included—then apply program policy and real-world context. That approach protects individuals from panic and helps programs build fair, defensible monitoring systems.
